Pharmacies across the nation are shutting down at an alarming rate, prompting advocates to raise urgent concerns about the implications for public health.
“We are observing not only a lack of access but also an increase in chronic illnesses, with more people visiting emergency rooms. This situation can lead to serious consequences, including fatalities,” stated Magaly Rodriguez de Bittner, Associate Dean at the University of Maryland School of Pharmacy.
“We’ve been stating that we are at a tipping point for quite some time, but the reality is that we have reached that point now,” said Stephen Wienner, owner of Mount Vernon Pharmacy. “I feel as though I’m sounding an alarm that no one is heeding.”
You may have noticed signs of this crisis in your neighborhood—boarded windows, sparse shelves, and locked parking lots where pharmacies once thrived.
In the past year, Rite Aid filed for bankruptcy, resulting in the closure of all its remaining locations. CVS also shuttered 270 stores nationwide as part of its restructuring efforts. Each corporate closure adds pressure to independent pharmacies that are already struggling to survive.
“Many of these closures are occurring in underserved areas where the local pharmacy is essential for community health,” DeBittner explained.
What was once viewed primarily as a rural issue has now spread to urban landscapes.
Currently, over 525,000 residents in Maryland live in areas experiencing a pharmacy shortage, accounting for approximately 8% of the state’s population, primarily affecting urban communities—70.3%—according to the University of Southern California’s Pharmacy Access Initiative, which monitors this growing concern.
Additionally, 38.1% of these shortage areas are classified as low-income.
IDENTIFYING THE SYMPTOMS
The term “pharmacy desert” refers to areas lacking accessible pharmacies. Urban residents without personal transportation are considered to live in a pharmacy desert if they are more than half a mile away from the nearest pharmacy. Conversely, for those in rural areas, that distance is defined as ten miles or more.
While the average American resides within five miles of a pharmacy, Rodriguez de Bittner points out that this distance is increasing. “We now see individuals needing to travel 10-15 miles just to fill prescriptions,” she remarked.
Tyra Walker, for example, has been forced to find a new pharmacy since her local option in Govans shut down last year. “It’s such a hassle,” Walker told WMAR-2 News’ Blair Sabol. “I used to walk there—it was just around the corner. Now, I have to take the bus to pick up my medications.”
Her concerns extend beyond her personal inconvenience. “Think about the senior citizens and those with mental health issues in this neighborhood. What options do they have?” she expressed.
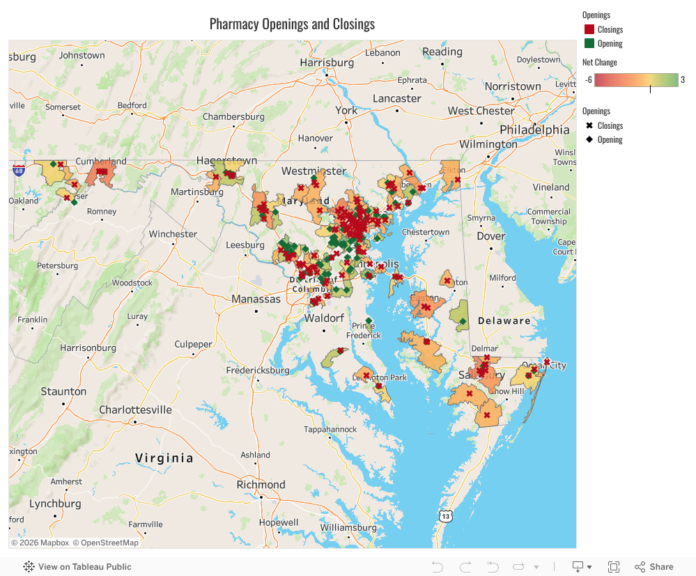
Records obtained by WMAR-2 News reveal the full extent of pharmacy closures in Maryland: over the past three fiscal years, a total of 156 pharmacies and distribution centers have closed, while only 97 have opened. These new openings often do not serve the areas most affected by closures.
The highest net loss of pharmacies occurred in the 21215 zip code in the Park Heights area, with six closures recorded.
 Tyra Walker has to take public transportation to pick up her prescriptions after her local pharmacy closed down last year.
Tyra Walker has to take public transportation to pick up her prescriptions after her local pharmacy closed down last year.UNDERSTANDING THE DIAGNOSIS
While some attribute the closures of certain pharmacies, particularly chains, to frequent shoplifting, advocates argue that the real culprits are the business models surrounding drug reimbursement, particularly Pharmacy Benefit Managers (PBMs).
Three companies—CVS Caremark, Express Scripts (Cigna), and OptumRx (UnitedHealth)—dominate 80% of the market. They dictate reimbursement rates for medications sold by pharmacies, and in recent years, these rates have continued to decline.
“We’re required to fill prescriptions for claims that are not profitable, until the business can no longer sustain itself,” Wienner noted. “We are easy targets in this scenario.”
“The contracts we receive are essentially take-it-or-leave-it,” said Eric Yospa, owner of Family Pharmacy in Hampstead, which he inherited from his father. “Some patients have been with us for over 20 years. Sometimes we simply can’t meet their needs because we lose $100 to $200 per prescription.”
Pharmacies are also hit with clawbacks, where PBMs reclaim a portion of the money after the insurance is processed. “This happens frequently, even though it shouldn’t,” Wienner stated.
After the closure of a hospital pharmacy, Wienner offered to take on some new clients, only with the understanding that it would be temporary. “Can you envision a business model where you have to say yes but also be prepared to vacate as quickly as possible? That’s absurd,” he emphasized. “It’s simply not sustainable.”
Earlier this year, Yospa severed ties with his pharmacy’s current PBM through its group contract, affecting many Medicare and elderly clients. “They will have to seek services elsewhere, and this transition isn’t ideal for anyone,” he noted. “They won’t receive the same quality of care they experienced here.”
Advocates are concerned that, without immediate action, the situation will worsen. “During the COVID pandemic, pharmacies were the backbone of healthcare, serving as a safety net,” Wienner added. “It’s unsettling because you only appreciate a safety net when it’s no longer there.”
POTENTIAL SOLUTIONS
At Yospa’s family pharmacy, they practice prescription compounding, which allows them to procure the active ingredients of medications that may otherwise be hard to source and customize them in the necessary formats for patients.
Wienner’s pharmacy utilizes robots to assist in counting pills and also provides specialized packaging and home delivery services for an additional fee. “If you ask me, we are now better positioned than ever to meet our customers’ needs, assuming we can survive,” he commented.
“We offer much more than just filling prescriptions and handing out bottles,” Rodriguez de Bittner emphasized. “We serve as accessible healthcare providers, playing a vital role in keeping communities healthy and reducing hospital visits.”
This year, emergency legislation has been introduced in the Maryland Senate to establish a minimum reimbursement floor for PBMs, particularly concerning Medicaid recipients. However, these proposals have repeatedly failed to advance out of the finance committee.
“From a legislative standpoint, the financial resources at play make major corporations look like small-time operators,” Wienner said.
“Unfortunately, money tends to dictate outcomes,” Yospa added. “As a result, patients bear the burden.”
In 2025, Virginia is set to implement legislation transitioning Medicaid to a single state-contracted PBM model, designed to ensure fair and consistent pharmacy reimbursements, as reported by the American Pharmacist Association. The same year, states like Indiana, Colorado, Iowa, Arkansas, and North Dakota adopted reforms targeting PBM practices.
This legislative session in Maryland raises questions about whether lawmakers will make another attempt. Instead, Rodriguez de Bittner asserts, “We are committed to convincing our legislators to take proactive steps before we reach a critical threshold.”
NURTURING THE NEXT GENERATION
At the School of Pharmacy, Rodriguez de Bittner emphasizes the importance of tracking pharmacy closures, especially for what she refers to as “keystone” pharmacies. These establishments play vital roles in maintaining the overall health of communities—like Wienner’s pharmacy, which specializes in care for patients with HIV and AIDS in Baltimore City.
The school is also addressing another pressing issue: the shortage of pharmacists to meet future demands for medical services. They’ve launched a unique program called “pharma-preneurship,” aiming to inspire the upcoming generation to become innovative problem solvers, emphasizing that the health of the pharmacy sector directly correlates with community health.
“We aim to empower young pharmacists with the tools to make a significant difference,” she concluded.